Since birth stories were one of my favorite ways to learn and get inspired for labor while I was pregnant, I now want to share my full story. Be aware, it’s a lengthy one, but it kind of has to be since my labor was quite lengthy as well.
Hypertension
My birth story must be prefaced by disclosing that I have chronic hypertension. Since my early twenties, I have a history of high blood pressure readings that can only be explained by family history, since both of my parents have hypertension although neither of them developed the condition so early in life. For at least five years, I’ve kept my blood pressure well under control through daily medication. It has been a well-known and easily managed condition. When we began trying to conceive last year, I switched to Labetalol, the most widely used blood pressure medication for pregnant women as it is safe for the baby, whereas many other medications are not.
Throughout the pregnancy, I knew that having chronic hypertension automatically classified me as a ‘high risk’ pregnancy and increased my risk of developing preeclampsia, a very dangerous condition that can result in excessively high blood pressure, seizures and even fatalities. But it wasn’t until about midway through the pregnancy that my doctor told me it’s a best practice to induce patients with hypertension 1-2 weeks early. At that point, I had been listening to the wonderfully educational podcast The Birth Hour religiously and I knew about some of the drawbacks to induction. Most importantly, I knew that I would strongly prefer to avoid induction and let my baby come naturally when she was ready.
As I progressed through the third trimester, my blood pressure continued to remain stable—excellent rather, with some of the lowest readings that I had seen in my adult life. The top number was often below 110 and the bottom number often in the 60’s. I began to truly question why an induction would be necessary without even a single high reading throughout the entire pregnancy. I asked my doctors if I could wait at least until my due date for induction, since there were no signs of anything going awry with my blood pressure. They agreed that was reasonable.
All of July I waited for baby Scarlett’s arrival (although at the time we didn’t know if she was a boy or a girl!), hoping that she would initiate spontaneous labor ahead of the dreaded induction date. About a week before my due date (7/28), I had my final doctor’s appointment and she was very firm about not wanting me to go past the due date. She felt that my risk for preeclampsia would rise dramatically each day after I was due. She checked me and reported I was 1.5cm dilated and about 50% effaced. I remained hopeful that I could get baby to come naturally. To me, the induction seemed preventative rather than at all medically necessary. I was walking at least 30 minutes every day, healthy, full of energy, and I would have happily waited another week. But, I am not a medical professional and this was my first pregnancy. Having chosen to go the OB / hospital route rather than seeking care from midwives in a birth center had set me up for this type of advice and conundrum. My husband, JB, was worried about the possibility of preeclampsia. I felt that I had already struck a compromise with them to not be induced early and decided I would go with the plan.
The induction was scheduled for Monday, July 29th at 5PM. In the days leading up to the induction, when it became more and more clear that baby wasn’t coming on her own I found myself in tears more than once. I knew in my heart I did not want to be induced, I was so sad that I was likely losing what might be my best chance at a more natural birth since I was already 33 years old and could only imagine that future pregnancies would be considered even higher risk. I was planning to attempt the delivery without the epidural and with as little medical intervention as I could. But I knew that inducing the labor would already lead me down a path of medical interventions, and everything I had heard about the intensity of Pitocin contractions made me very much aware that I might end up needing the epidural.
The Induction
So we arrived at the hospital, Monday at 5PM after a ‘last meal’ of burgers, fries and an Oreo milk shake from The Habit. The ‘stork’ labor & delivery parking spaces outside Kaiser South Bay were nearly full, leading me to believe that it was likely a busy evening for births. We waited in the waiting room for nearly a full hour. Right at 6PM, just as I was beginning to hope they needed us to reschedule, a medical assistant came out and led us through the doors, to our room that was ready and waiting. I disrobed into a hospital gown and offered my wrist for the placement of an IV lock, transitioning from a healthy pregnant woman to the status of hospital patient. I was promptly hooked up to the wireless monitor, as I had requested so that I could remain mobile. This showed the baby’s heart rate and monitored my contractions. To our excitement, the monitor showed that I was having regular contractions that I couldn’t feel. I was hopeful that this meant I had progressed and was perhaps closer to active labor than I had thought. Soon after, I was checked for dilation and effacement—then received the disheartening news that I was still 1.5 cm dilated and 50% effaced, despite partaking in all the natural induction remedies that I could and feeling some cramping.
At 7PM, they commenced with the first induction procedure—the placement of a foley catheter bulb which was supposed to dilate my cervix to 4cm, or stay in for 12 hours–whichever happened first. The placement procedure was more uncomfortable than I had imagined it would be. They had to find the 1.5cm opening of my cervix and get the angle just right in order to insert the catheter, unfortunately that took a few tries. My husband said that it seemed pretty quick to him but to me it took forever. It was probably 5 minutes, but that’s a long time to have a foreign object manually twisted around into your tiny cervix. The doctor commented that I must have a high pain tolerance, as she had seen many patients scream in agony at the placement of the balloon and all I did was silently breathe through it. I was hopeful that was true and that I could get through my contractions with my natural endurance.
Once it was in place, we waited. It wasn’t the most uncomfortable thing, but it did exert a constant pressure that made it kind of hard to sleep that night. The medical team offered to start my Pitocin that night—I guess it’s common practice—but I hadn’t been anticipating that, and some small part of me was still hoping that I could get labor into swing without the chemical so I refused.
By morning, I was starving and patiently awaiting a cervical check. Much to my dismay, the balloon hadn’t fallen out on its own, which I knew meant that I was definitely not 4cm. Since I had declined the Pitocin, my nurses said that it was still ok for me to eat. So I excitedly ordered breakfast from the hospital menu—an English muffin with jam, cheesy potatoes and fruit. My balloon removal and cervical check revealed that I was still 1.5cm but that I had increased my effacement to about 70%. Not quite the progress I had hoped for in my first 12 hours of labor. The next step was to start the Pitocin, I was in for it now, it was unavoidable.
The Reign of Pitocin
At 10AM my IV drip began and I hoped for the best. The nurses advised us that the baby was usually born about 24 hours after Pitocin was started during most inductions, so we shouldn’t expect to progress super quickly. I tried moving around to get the baby to descend. We took a walk around the halls and said ‘hi’ to the friendly ultrasound tech who had helped with my non-stress tests. I sat in the rocking chair and bounced on my birth ball. We started listening to the birth playlist I had created. Every half hour the nurses would come in, check my contraction progress and increase the dose of Pitocin by 2. It wasn’t until around 12 or so that I began to actually feel the contractions that told a rhythmic, abstract story on my hospital monitor. They felt gentle at first, simple a tugging that coincided with the peaks that I observed on the monitor, although the monitor did have a delay of several seconds from what I was feeling.
It was around this time that I started to use some of the LaMaze techniques that we had learned through Kaiser’s Prepared Childbirth course. I preferred the long, deep breathing technique so I started practicing it when I felt each contraction begin. I had been walking around and moving quite a bit, so around 3:10 I decided to take a seat on the bed and rest a little as I knew I might not get another chance if the contractions ramped up. JB ran out to the car to get something—neither of us can remember exactly why he left or for what, just that he wasn’t there when I was sitting on the bed around 3:15PM and I felt the warm, uncontrollable gush of amniotic fluid between my legs. I sat in the oozing puddle, heart pounding excitedly, knowing that this must be my water breaking. I was thrilled that it broke naturally, and thought to myself that maybe I was approaching active labor—it certainly seemed like something was happening, I had to be progressing.
The frequency of my contractions was increasing, and shortly thereafter the nurse came in and went to turn down my Pitocin level—which had been up to 16. She explained that my contractions were a bit more frequent than they like to see—they want to see established, rhythmic contractions but with more of a break between them. I thanked her and told her that I thought my water had broken. JB walked back into the room, right as the nurse went to get the test kit.
“Babe, I think my water broke!” I exclaimed.
“Really?” He was excited, but a little disappointed that he had been out of the room during such a big milestone in labor.
“Yep, it’s amniotic fluid. Your water has broken, and it’s clear—no meconium in the fluid.” The nurse announced, sharing our joy at the progression of my labor.
She helped me into the bathroom and helped me clean up the strange mix of fluid and blood that was seeping out of me, handing me a pair of mesh hospital underwear and the largest pad I had ever seen. It was so massive I wasn’t sure how it would even fit in the underwear, it was as long as a puppy pad!
“I hate to tell you this but there’s going to be a lot more of this—it’s going to get messy so don’t worry too much about trying to keep clean.” She advised me. At that point, she also let us know that she and the anesthesiologists were about to commence surgery for my neighbor’s C-section. She warned me that should I want the epidural I should ask for it early, before the pain became insurmountable, since I might have to wait up to an hour for the anesthesiologists to finish surgery. I felt like I was managing my pain well, but thanked her for the heads up.
Being on the toilet was comforting, it felt like the perfect place to embrace the intensifying contractions and expulsion of fluid as each one swept over me. I crouched over the toilet and held JB, breathing slowly and intentionally for each one. Between contractions, I quickly taught him how to count with me as I had been in my head to ease the pain, the counting helped me feel in control and as if I knew when the pain would start subsiding. I counted as if it were musical bars, 1-2-3-4, 2-2-3-4, with each bar being a breath in, and the next being a breath out. I knew that by the time I got to the 7th bar the contraction was pretty much over. The focus helped distract from the massive swells of discomfort that hadn’t seemed to be quelled by the nurse turning down the Pitocin.
We were in this—they were lasting about 60 seconds with only a 60 second break between each one. If JB wanted to leave to grab something or we wanted to move / change positions, I insisted that this happen immediately after a contraction to minimize the chance of not being ready or in an optimal position when the next one began. We moved around, from a couple positions in the bathroom, to leaning over a counter in the hospital room, to the slow dancing / swaying position and to the rocking chair. But the sheer volume of contractions that showed no signs of slowing was incredibly exhausting. I was covered in sweat and while I had confidence that I could get through each one, I knew that I did not have the endurance to do this all night. The breaks were just too short. It was impossible to get much solace as I was immediately gearing up for the next inevitable wave of pain. When I had last been checked I was 1.5. The outlook didn’t seem good for a quick delivery, even though the intensity—both physically and mentally–was unparalleled to any other situation I had been through in my life. I found myself wanting an escape. As much as it helped to move around through each contraction, my thoughts drifted more and more to the bed and how nice it sounded to just lie back and relax, like the stories I had heard of women who got the epidural, to get some relief and relax my muscles. I thought of what the nurse had said about the anesthesiologists and what they had told me when the process began—that while it was never technically too late for the epidural, they could not administer it unless you were perfectly still. And some patients waited to the point where they could not stay still through the contractions.
I told JB I was thinking about it. He knew that I was hoping to go through the experience without it, so he suggested that we take a walk out into the hallways before I ask for it. A walk sounded like something that I absolutely couldn’t do. I would have to stop so frequently to sway and breathe through the contractions, and without anything but him to lean on. And I’d have to deal with lugging the IV machine and trying to avoid the cords. It was way outside of my comfort zone, which was slowly shrinking in around me as the hospital room transformed into a world of pain. I told him I wasn’t going to be upset with him for letting me get it, I told him that there was no way I could do this all night. I wasn’t sure how close I was but I knew that nothing sounded better than getting on that bed and finishing my labor there. Seeing how serious I was, he relented and guided me to the bedside phone to call for help.
In retrospect, perhaps we should have considered the analgesic medications at this point. Especially if I was still not very far along, which I suspected. But I knew that they brought only temporary relief and that once you got one dose you usually wanted another. I just wanted to go for it, the epidural loomed in my mind as the golden ticket to relief. I also wonder if perhaps I should’ve asked to be checked first, but I honestly just did not want to delay the process of getting on that anesthesiologist’s to-do list.
The Bed
“Hello, I’d like to request the epidural,” I remember speaking politely, although my voice probably sounded a bit strained. I tried not to think too urgently, it could be a while before they could help me. But at least I had initiated the process, at least help was on the way.
It was 5:45PM when the anesthesiologist arrived in my room to administer the epidural. JB was instructed to leave the room. None of my reasoning for resisting it seemed to matter at all anymore, the only thing that mattered was finding a way out of the cycle of torturous swells of pain. I never knew I could appreciate anyone’s career choice so much, I didn’t know how I could ever thank him enough for having the tools and knowledge to get me through this.
They told me that I’d have to be completely still. I needed to tell him when the contraction was starting, but not to move at all. I said I could do it. It was a monumental challenge, since I had been relying on movement to ease the pain for hours, but I was up for it if it meant the end was in sight.
I remember the song ‘Crash into me’ was playing from my playlist, and he asked me if I was a Dave Matthews fan, I think because he was. “Yes, well, I like this song. I like what I know of his songs, but I don’t know a lot. I’m not a huge fan.” I stammered, not knowing how to properly describe my relationship with the Dave Matthews Band exactly at that moment. I leaned forward and meekly told them a contraction was beginning. Then I sat perfectly still, as I knew that there was some tiny little needle making its way toward my spinal cord and that any movement I made could really screw things up for me. I felt like I was playing dead, trying to pretend like the pain that I felt wasn’t real. That I was somewhere far above and away from the little room and the small pain ridden body that I was in.
The process was fairly quick. It was only 3 or 4 contractions until I began to feel some relief. He told me that it would take about 20 minutes to fully take effect and that it wasn’t supposed to numb the pain completely, it was just supposed to make it manageable and allow me to relax my muscles. That sounded great to me. And slowly, my muscles released and I sunk back into the hospital bed—probably for the long haul, although I still didn’t know just how long.
It was probably an hour or so later. Before 7PM I think, that the nurses came back in to check my progress.
“You are still at 1.5 centimeters, but fully effaced.” The nurse delivered the mind-boggling words of crushing disappointment. How was that possible?? My water had broken, my contractions had intensified to the point that I couldn’t use my LaMaze techniques to get through them anymore, they were practically back to back, and at one point when feeling nauseous I had actually wondered if maybe I might be nearing transition. Yet, what they were telling me was that all that I had experienced was technically only ‘early labor.’ I was not even in active labor. After being told I had a high pain tolerance, then encountering the freight train of cascading, unwavering, ripping agony right through my midsection for hours, I hadn’t progressed to active labor. I didn’t fully buy it. The Pitocin threw everything out of its natural order and I still refuse to fully accept that what I experienced doesn’t count as active labor. I will never let my lack of dilation disparage the pain that I experienced, because it was incredibly real. I guess if what I was in was early labor, then I never want to experience active labor. I think that Pitocin labor doesn’t really match up to the metrics for what would occur naturally. My body and my baby were fighting it, despite my efforts to power through.
The silver lining was that I had absolutely made the right choice in getting the epidural when I did. I will never doubt my decision to do so. I would have never made it through an entire night of that hell. I think JB and I would have both devolved into madness.
The next time they checked me—a couple hours later—I was ‘between 3 and 4’ according to the nurse. It was at this point that I began to doubt that the induction was going to work. All that and no progress? At what point do we throw in the towel and opt for the C-section? I could feel myself nearing that point, I was not afraid of it if it was necessary and if I couldn’t progress I assumed it may become necessary. That night, my doctor was on shift and she came in to talk to me. She was still optimistic about the induction and the possibility of a vaginal delivery. She said that as long as I progressed through the night that there was a good chance of it.
The next 12 hours—the part where I supposedly went through the ‘active’ part of my labor were spent on the bed, trying to get comfortable and shift the dead weight of my legs back and forth so as not to spend too much time in one position and possibly injure myself since I couldn’t fully feel whether I was in pain on my lower body. I remember also feeling a pressure in my rib cage that I had not felt before. It seemed unusual, since baby was supposed to be descending and I hadn’t felt her kick my ribs at all the entire pregnancy. I squirmed to try to alleviate it, but she was persistent.
I was able to get some sleep that night, although it was very light, troubled, and hungry sleep. The contractions were not fully gone although the epidural kept the intensity of the pain at bay. I remember that the growing hunger in my stomach added to my discomfort and was beginning to make me feel weak, I was glad that I wasn’t still trying to labor with my energy levels running on empty.
I’m fortunate that I was in a state of drowsiness and not fully able to understand the scare that happened around 3am that night. My baby’s heartrate plummeted after I shifted to my right side—her heart rate was down into the 40s for more than 4 minutes and all the medical staff on the floor were gathered in our room. JB tells me he woke up and realized what was happening, that there was a crisis going on. I have no memory of this, just that they wouldn’t let me stay on my right side. They were about 30 seconds away from taking me in for an emergency C-section, when her heart rate climbed back up and stabilized in the normal range. Thankfully.
Stage Two / Terrapin Station
I think I was checked twice during the night, once I was ‘5-6’ and the next time ‘8-9.’ By 7AM, when the shift was changing, the night nurse checked me one last time and declared me complete. It seemed incredulous that I had gone through such a monumental opening and even through transition while barely feeling a thing. I was ready to push, but they weren’t really in a hurry to have me start, I’m not sure why. They brought in a kit with tools to prepare for baby’s arrival. A new team of nurses came in, one with 35 years of experience who was actually retiring the next week. It wasn’t until 9AM that they got me in position to push and so it began.
I could feel and move my feet, but not most of my legs so I relied heavily on the help of JB and the nurses to move my legs into position, and then to help hold them up as the process began. I was instructed to start pushing when I felt a contraction beginning, and to push hard for a 10 count, holding my breath, then release to grab another breath and repeat. For each contraction, they said I should do this 3-4 times. While I could still feel the tightening of the contractions, it was impossible to tell if it was going to be a big one or just a small blip on the monitor. And sometimes my desire to push tricked me into thinking that one was starting when it wasn’t. They wanted me to take breaks between the pushing to regain my strength. It was really up to me to know when to push though because it would take at least 5 seconds for the monitor to reveal what was happening, so I couldn’t rely on them to tell me when.
It was challenging, they told me to make sure I was push all the way through and bearing down—as if I was taking the biggest poop of my life. I was not supposed to hold any of the pressure in my face, but when you’re holding your breath it’s tough not to. They told me I got the hang of it, and that I was pushing correctly—especially since I pushed out 3 stools during the first hour or so! It was a whole new level of intimacy with JB, he had never seen me poop before and I can only imagine how raw and completely unsexy his view of my nether regions was. But it didn’t bother me in the slightest, I knew how common it was to poop during pushing and I had mentally prepared for it. My only goal at that point was to get this baby out and into the world. We were ready.
Despite pushing correctly, Scarlett didn’t seem to be descending. When we started I was told she was in a +2 station, meaning her head was above the pelvis still. And I knew that she couldn’t have moved that much because I continued to feel an intense pressure in my left ribs. I was sure that the balloon, and the cervical checks and the hands had prompted her to retreat as far up into me as she could. She was jammed up in there and no amount of external nudging with the nurse’s hands and mom pushing could dislodge her. The nurse could feel her body at an odd, diagonal angle through my abdomen. Despite being head down, her position was not ideal for a trip through the vaginal canal as she was sort of twisted diagonally across my abdomen. We all remained optimistic that I could do this though, that I could deliver a healthy baby vaginally after a multi-day labor. But the clock kept progressing, and baby did not.
I felt like I needed to have gravity working with me instead of against me as it seemed to be. That was the big drawback to the epidural, I couldn’t squat or easily get into a hands and knees position where gravity could help coax her out. The nurses came up with a couple of different positions that I could try without having the use of my legs, we used a sheet around a labor bar so that I could lean upward into more of a sitting position. But, the morning wore on and nothing we tried seemed to help. I kept hoping I would hear them say that they could see the head or some other real sign of progress besides just encouraging words. Throughout the pushing amniotic fluid streamed out of me from time to time, and unlike when it first appeared on Tuesday afternoon, there was now meconium present in the fluid. Everything that had transpired had likely stressed the poor baby a bit, and she had passed her first stool just in the last few hours. It wasn’t a big deal, but it made me sad to think of her distressed and resisting.
It was 12PM when the midwife came in and declared that her position was still +2, after 3 hours of pushing. I had heard in other birth stories that people are often not allowed to go past 2 hours, but they were being generous in allowing me the time to try to get her out before resorting to surgery. They told me I could try until 12:30 and then they were going to have to call it unsuccessful, and we would go to the operating room. The deadline made me try even harder—the pushing actually felt really good too. It was a relief and pushing into the contractions seemed to counter the power of their pain. It felt natural, and as each contraction came, I continued to push. It couldn’t hurt since I was 10cm—even though it wasn’t getting me anywhere.
First Birth, Second Surgery
At 12:45, Dr. Lopez came in and introduced himself and I signed some paperwork. He explained that C-sections were generally safe but came with some risks, that the major difference with a C-section delivery was the price, but there wasn’t really another option at that point. She was too high for a forcep or vacuum assisted delivery. The team that would be performing the surgery had a cumulative total of about 150 years of experience. I was in good hands and I knew they did this every day, multiple teams per day, as they had done with my neighbor only hours earlier.
This is the part where I feel like my previous surgery experience really helped me to keep a positive attitude—I really was not afraid at all. I was a little disappointed that after so many hours of labor it was going to end in a C-section, since I could’ve just scheduled one and avoided all the pain and drama. I wasn’t really looking forward to having another scar on my abdomen, and having future deliveries be complicated by a previous C-section, but I was not fearful. It wasn’t ideal, but I definitely understood the necessity of it after all the exhaustion, the hunger, the pain. We were beyond ready to meet her and she needed to come out, despite her stubborn inclination to gravitate toward my ribs.
JB was instructed to put on his scrubs and wait outside, and I was wheeled into the operating room where the team prepared for surgery. Since I already had the epidural in place, it was just a matter of some additional medication to further numb my abdominal area. They put up a blue curtain, and I was surprised at how close to my face it was. It was so odd to be awake for all of the busy, perfunctory medical preparations and small talk amongst the staff that typically occur when the patient is placed under anesthesia. I remember being cold, so cold. The blankets they put over my shoulders and arms didn’t seem to help. I was shivering. It’s a normal affect of the medicine, they said. It didn’t make it less uncomfortable.
JB had been outside waiting—I later found out for about 30 minutes! It didn’t seem that long to me. He was trying to keep our closest family members updated about the situation as we kept getting tons of messages from people who knew that we had checked into the hospital on Monday, since it was now Wednesday afternoon. The doctors finally brought him in. He asked if he could watch, but they advised him he should be with me. We held hands as the surgery began. It was just like I had heard it described by so many, just the sensation of tugging. No pain.
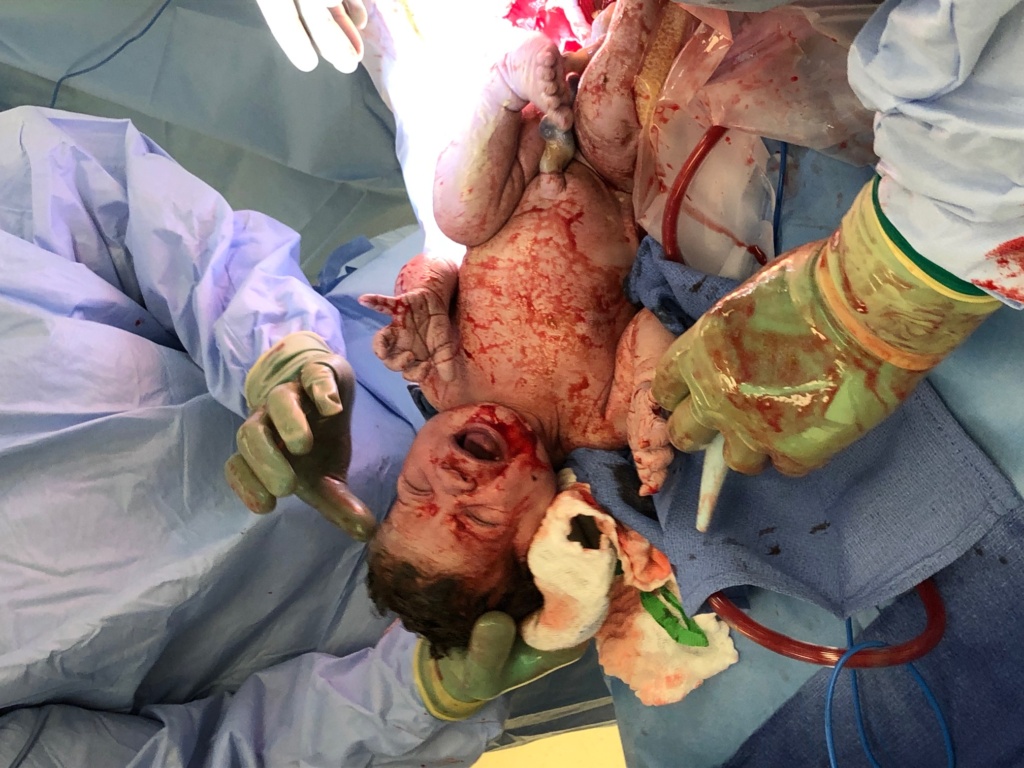
Then we heard it—the loud, livid cries of our baby! She certainly came out with fully developed lungs and a strongly emotive voice she knew how to use. They told him he could go take pictures, so he excitedly ventured to the otherside of the curtain where he saw a gory mess of blood and a baby girl with a red, scrunched up angry face and a head of thick brown hair!
“It’s a girl!” JB exclaimed, bringing to a close our 9 months of waiting, wondering, hypothesizing and flip flopping.

They quickly suctioned her lungs (since meconium had been found in her fluid) and performed some initial screenings. Daddy stayed with her during that and cut her cord, I knew right away that she was going to be a daddy’s girl forever. They brought her to me when they could although we didn’t have the ideal skin to skin golden hour experience that we had been planning. It was frustrating to not get to see her right away when she emerged, or to have her immediately plopped onto my chest while we were still connected via umbilical cord. But it was nice to hold her when she was so fresh and so tiny! I remember she looked at me with her big eyes and the three of us shared an embrace, and our first family photo. I was in awe of her and couldn’t believe everything that had transpired. They told me her apgar scores were 8 and 9 respectively, he told me “we never give tens anymore,” so she was basically as healthy as could be. She clocked in at 7 pound, 13 ounces and measured 20 and a half inches in length. The doctors sewed me back up and after a short while we were brought to the recovery room. There, we had some family bonding time and she got a chance to nurse for the first time. I was amazed at her inherent knowledge of how to latch and suck. My breasts didn’t feel it with near her level of intuition.
“Penelope?” JB asked me, since that had been our frontrunner name for a girl for months.
I shook my head.
“Scarlett,” I said, “I started thinking of her as Scarlett immediately.”
It was a name we had both agreed upon later in the pregnancy. I thought it was beautiful, and I found out later that he had suggested it because of the Grateful Dead song Scarlet Begonias. Which hadn’t even crossed my mind, but I am happy now that there is a song associated with her.
There is so much more to be said, about the recovery, the breastfeeding experience, and the challenge of the newborn weeks—but that is the story of Scarlett Genevieve Brown’s birth. It was a long one, but she was born before July could end and she is nothing short of the gorgeous, long-haired summer baby that we had dreamed of.

0 Comments
1 Pingback